Mental health disorders are complex and often misunderstood. And these two are among the least well understood and most often confused. In fact, there is a lot of controversy surrounding the relationship between borderline personality disorder (BPD) and multiple personality disorder (MPD/DID).
MPD is now known as Dissociative Identity Disorder (DID). It was once more commonly referred to as Split Personality Disorder.
Diagnoses between the two are often very difficult. Research indicates the disorders have some distinguishing features but also considerable overlap as both have some similar symptoms.
Is BPD the Same as Multiple Personality Disorder?
Emotional dysregulation is a core feature of both BPD and DID. Some research suggests BPD patients grow up in homes in which overtly expressed aggression is more tolerated, or at least more openly experienced. DID patients grow up in homes in which the fact of aggression is kept a secret. This has consequences for the formation of psychic structure in each disorder.
People with BPD have great emotional instability, impulsive behavior, and fear of abandonment. Symptoms include intense emotions, unstable relationships, and self-destructive behavior. Causes include genetic factors, childhood trauma, developmental deficiencies, and neurobiological issues. Treatment usually involves Dialectical Behavioural Therapy (DBT), medication, and appropriate support systems.
DID is a complicated mental illness that leaves its victims with enduring memory issues, behavioral abnormalities, and identity difficulties. People with DID frequently have two or more (often many) distinct personality identities, each with its memories, characteristics, and attributes. They often switch between their identities, have extensive memory gaps and feel disconnected from themselves.
Other symptoms of DID may include headaches, trances and out of body experiences. There is a high correlation with severe childhood traumatic events, especially sexual trauma. It is believed to develop to help people avoid unpleasant or traumatic memories.
Because of its complexity, symptoms of DID are explained in this table.
| Category | Symptoms |
| Dissociation | Memory gaps or amnesia – feeling detached from oneself – out-of-body experiences |
| Identity alteration | Presence of two or more distinct personalities or identities – differences in voice, mannerisms, and even physical characteristics between identities – each identity might have its own name, personal history, and characteristics |
| Memory symptoms | Amnesia for personal information – inability to recall key personal events, traumatic or not – finding unfamiliar objects or writings among personal belongings |
| Depersonalization | Feeling that the world is strange or unreal – feeling like an outside observer of one’s life |
| Derealization | feeling that the environment is strange or unreal (objects seem distorted; time may seem to slow down or speed up) |
| Emotional symptoms | Sudden emotional shifts – feeling numb or muted emotions – experiencing sudden anger, sadness, or other emotions without a clear cause |
| Somatic symptoms | Experiencing physical pain or other symptoms without a clear physical cause – phantom sensations, such as feeling as though one has a different body |
| Other symptoms | Hearing voices inside one’s head (that may be perceived as coming from another identity) – engaging in behaviors that are out of character, and not remembering them later- trances or “zoning out” |
What Is the Difference Between BPD and DID – and How Do You Get Diagnosed?
Borderline personality disorder can be a difficult diagnosis because of its similarities to other conditions, particularly mood disorders. Women account for 70% of patients with this disorder in clinical settings, and the most common age of onset is in late adolescence, most commonly following threatened suicide or a suicide attempt. Common diagnostic criteria and processes for BPD, including psychiatric interviews and the DSM-5 guidelines, are simply presented here.
To get diagnosed, the first thing you should do is see a medical professional. Typically they will talk with you about your symptoms, physical health, and past and present life situation. They may ask you to complete a questionnaire about your symptoms as well as meet with a family member. Because BPD often co-occurs with other mental health conditions, they need to rule those out to come to a diagnosis and then discuss it with you.
Getting Diagnosed with DID
Finding an appropriate mental health professional for a diagnosis of DID may be challenging and require patience while navigating the mental health system. Getting diagnosed for DID takes time, often at least 7 years, due to the many similar or co-occurring diagnoses that need to be sorted out. Diagnosis focuses on the importance of recognizing distinct identities and recovering memories during assessment. Many people who have DID also have borderline or other personality disorders, depression, and anxiety, further complicating the diagnosis.

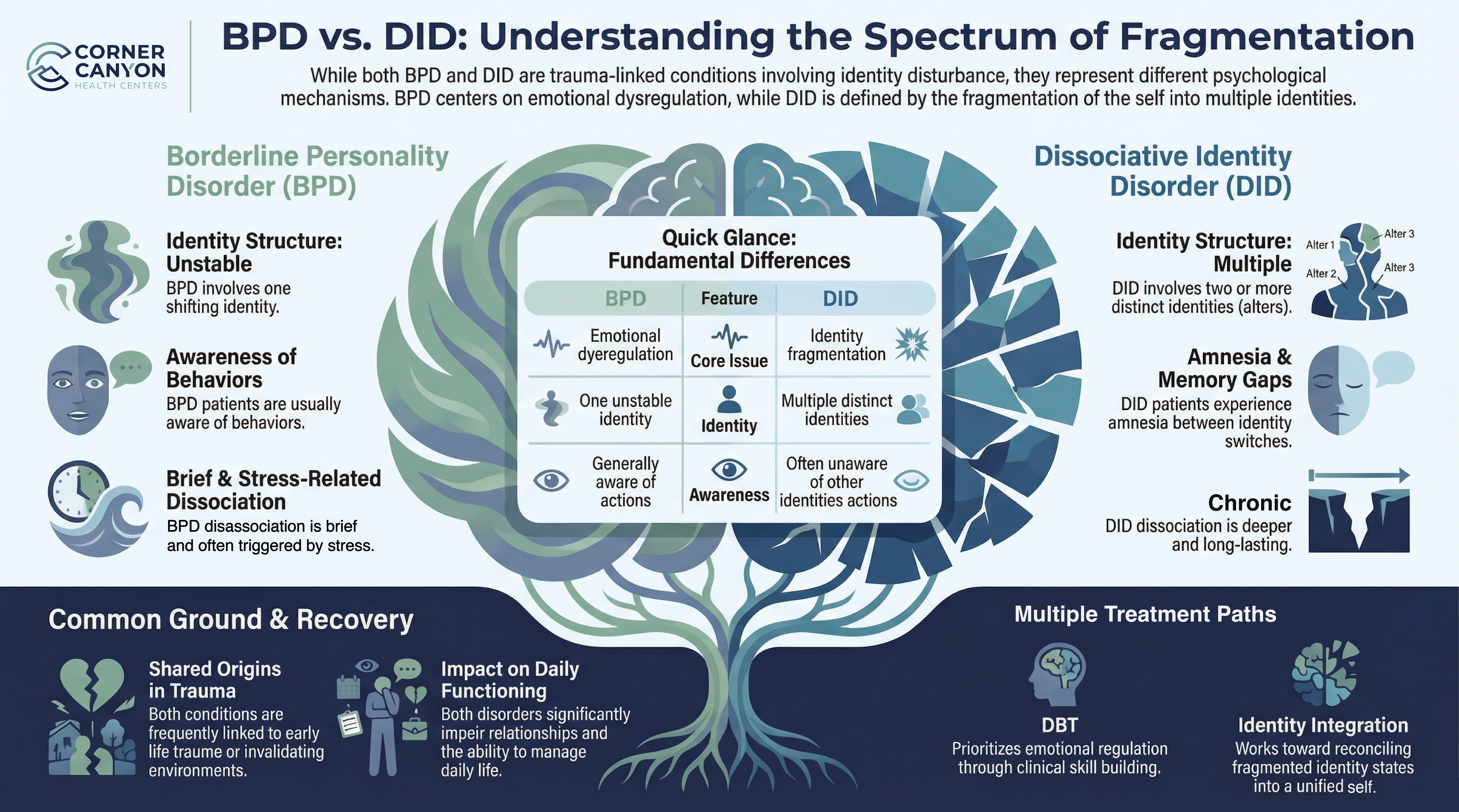
Key Differences Between BPD and DID
Trauma specialists think that trauma is typically the underlying cause of both borderline symptoms and DID.
Nature of Identity
BPD: Characterized by a single, unstable self-identity, leading to frequent changes in self-image and goals.
DID: Involves the presence of two or more distinct identities or personality states called “alters”, each with its own way of perceiving and interacting with the world. They control the behavior at times. Generally there is a “host” personality that identifies with the person’s real name but is usually unaware of other personalities.There is a lack of connection in memories, thoughts, feelings and actions.
Emotional and Behavioral Patterns
BPD: Marked by intense emotional fluctuations, impulsivity, and an overwhelming fear of abandonment. Individuals may experience rapid mood swings and unstable relationships.
DID: Defined by identity switching, memory gaps, and dissociative episodes. Each identity may have distinct behaviors, memories, tastes and preferences.
Diagnosis and Misconceptions
BPD: Common misconceptions include beliefs about manipulative behavior and unpredictability. BPD is often stigmatized for its emotional instability.
DID: Misunderstood due to Hollywood portrayals, leading to false beliefs about the nature of multiple identities. Reality is more complex and involves distinct identity states formed as a defense against trauma.
What Causes Personality Disorders?
Personality disorders are complex mental health conditions influenced by a combination of genetic, environmental, and developmental factors. Understanding the causes and triggers can help clarify why symptoms develop and guide effective treatment.
Causes and Triggers of BPD
Individuals with BPD may have a family history of mood disorders or emotional dysregulation, making them more susceptible to developing the condition. Childhood trauma, including neglect, emotional abuse, or unstable family dynamics, can significantly increase the risk. Additionally, repeated experiences of abandonment or unstable relationships may reinforce emotional instability and impulsive behaviors seen in BPD.
Causes and Triggers of DID
Dissociative Identity Disorder (DID) is strongly linked to severe, chronic trauma during early childhood, such as physical, emotional, or sexual abuse. In response to overwhelming stress, the mind may develop distinct identity states, or “alters,” as a coping mechanism to compartmentalize painful memories and emotions.
These dissociative responses help the individual survive the trauma but can lead to significant memory gaps, identity confusion, and difficulties in emotional regulation later in life. While trauma is the primary factor, other influences such as genetics, attachment disruptions, and environmental instability may contribute to the development of DID.
Common Treatments for BPD and DID
BPD Treatment
Treatment approaches for BPD typically involve Dialectical Behavior Therapy (DBT), psychotherapy, and medication for symptom relief, usually antidepressants. DBT was developed primarily to treat BPD by developing healthy coping skills to replace unhealthy behavior. It is a type of cognitive behavioral therapy (CBT) that teaches you how to be present and also provides skills using mindfulness for coping with stress, emotional regulation, and relationship improvement
DID Treatment
While there is no single evidence-based treatment for Dissociative Identity Disorder (DID), a variety of approaches can help individuals manage symptoms, integrate identities, and lead productive lives. Treatment typically focuses on long-term, trauma-informed psychotherapy that addresses underlying trauma and supports the integration of multiple identity states.
A key therapeutic approach is Internal Family Systems (IFS) therapy, which helps individuals explore and harmonize distinct identity states (“alters”) in a safe, structured way. This approach encourages cooperation among different parts of the self and promotes emotional healing.
Cognitive Behavioral Therapy (CBT) can be used alongside IFS to address negative thought patterns, anxiety, and depression, while grounding techniques help individuals stay present and reduce dissociation. For co-occurring symptoms, medication management—including SSRIs or anti-anxiety medications—may be recommended.
Additional supports, such as group therapy, provide peer connection and skill-building opportunities, and family therapy can educate loved ones and strengthen the patient’s support system.
Psychiatric Treatment for BPD and DID in Utah County
If you or a loved one are struggling with borderline personality disorder (BPD) or dissociative identity disorder (DID), Corner Canyon Health provides comprehensive care tailored to your needs.
Our services at Corner Canyon Health provide inpatient treatment for acute stabilization for individuals experiencing self-harm behaviors or suicidal thoughts, ensuring safety during crisis moments. Following stabilization, we offer ongoing outpatient support, including DBT, psychiatric evaluations, and medication management, helping you build emotional regulation skills, maintain stability, and achieve long-term mental wellness.
Schedule a consultation today and take the first step toward healing.
Frequently Asked Questions
What does MPD stand for?
MPD stands for Multiple Personality Disorder, which is the former term for what is now called Dissociative Identity Disorder (DID). While the name has changed, the condition involves experiencing two or more distinct identities or personality states, each with its own memories, behaviors, and ways of interacting with the world.
What Is DID?
Dissociative Identity Disorder (DID) is a complex mental health condition often linked to severe childhood trauma. People with DID may experience memory gaps, identity switches, dissociation, and emotional dysregulation. Proper treatment involves specialized therapy, psychiatric evaluation, and sometimes medication to support long-term stability and mental wellness.
What’s the difference between BPD and DID?
Borderline Personality Disorder (BPD) primarily involves intense emotional instability, impulsive behaviors, and fear of abandonment, usually with a single, unstable sense of self. DID, on the other hand, involves multiple distinct identities, memory gaps, and dissociative experiences. While both can be triggered by trauma, treatment approaches differ, with BPD often responding to DBT and therapy, and DID requiring long-term trauma-focused interventions.
How does Corner Canyon Health in Utah County help patients with BPD or DID?
At Corner Canyon Health in Utah County, we understand the unique challenges and stigma surrounding BPD and DID. Our compassionate care team provides a judgment-free environment and advanced, evidence-backed treatment, combining inpatient stabilization and ongoing outpatient support. We focus on helping patients manage emotional distress, develop healthy coping skills, and achieve meaningful recovery at every stage of care.
What specialized treatments does Corner Canyon Health offer for BPD?
Our BPD treatment is designed to address the complex emotional challenges and underlying trauma associated with the disorder.
We provide Dialectical Behavior Therapy (DBT), a proven approach that teaches skills for emotional regulation, distress tolerance, and healthy relationship management. In addition, group therapy sessions create a supportive environment where patients can practice coping strategies and gain connection with others facing similar challenges.
Our team also focuses on exploring and addressing underlying trauma, ensuring a comprehensive, individualized plan that promotes long-term stability.
Sources
Marmer S. and D. Fink. 1994. Rethinking the comparison of borderline personality disorder and multiple personality disorder. Psychiatr Clin North Am. 1994 Dec;17(4):743-71
Saxena M. et al. 2023. Multiple Personality Disorder or Dissociative Identity Disorder: Etiology, Diagnosis, and Management. Cureus 15(11): e49057. doi:10.7759/cureus.49057
Biskin R and J. Paris. 2012. Diagnosing borderline personality disorder. CMAJ. 2012 Nov 6; 184(16): 1789–1794. doi: 10.1503/cmaj.090618
Salters-Pedneault, K. 2023. BPD Criteria for Diagnosis. Borderline Personality Disorder in the DSM-5. Verywellmind.
